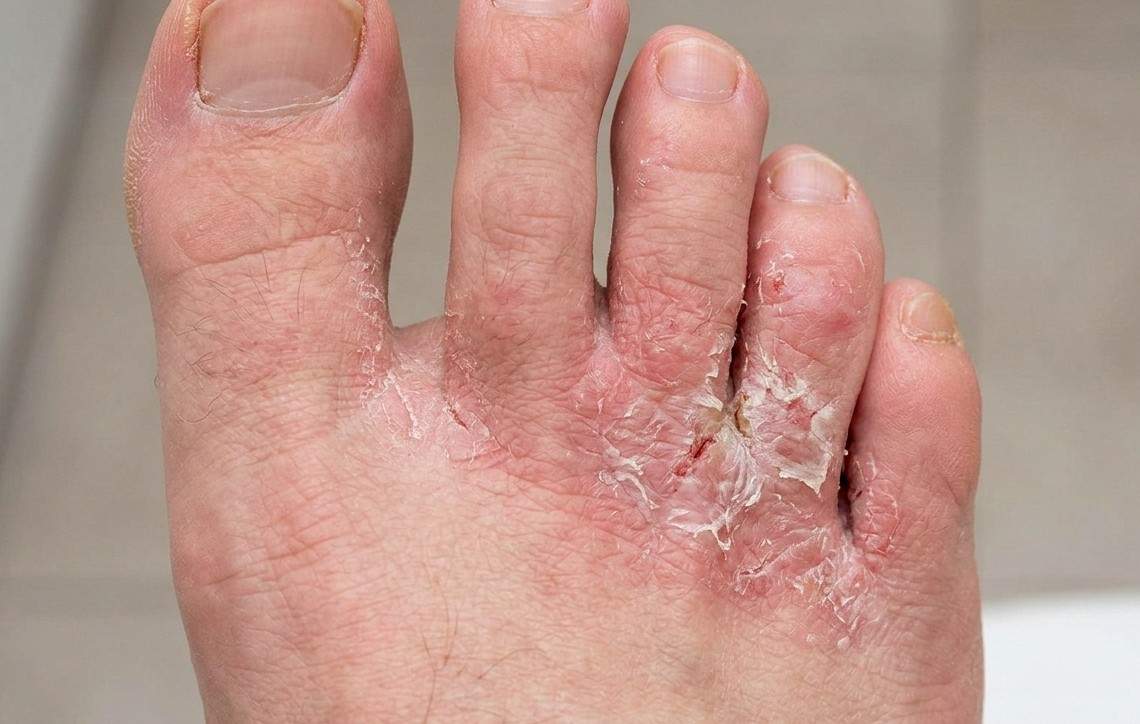
Athlete’s foot is one of the most common fungal skin infections worldwide. Despite its name, you don’t have to be an athlete to get it. Anyone can develop this itchy, irritating condition, especially in warm and humid climates or if they frequently wear closed shoes for long hours. In this guide, we’ll explore what athlete’s foot is, what causes it, how to recognize the symptoms, available treatment options, home remedies, prevention strategies, complications, and when to see a doctor.
What Is Athlete’s Foot?
Athlete’s foot, medically known as Tinea pedis, is a contagious fungal infection that affects the skin on the feet. It most commonly appears between the toes but can also spread to the soles, sides, and even the toenails. It belongs to a group of fungal infections called “tinea” infections, which also include:
- Tinea corporis (ringworm of the body)
- Tinea cruris (jock itch)
The fungi responsible for athlete’s foot thrive in warm, moist environments—such as sweaty shoes, locker rooms, public showers, and swimming pool areas.
What Causes Athlete’s Foot?
Athlete’s foot is caused by fungi known as dermatophytes. These microscopic organisms feed on keratin, a protein found in the outer layer of skin, hair, and nails. Common causes and risk factors:
- Warm, humid conditions: Fungi multiply quickly in moist environments.
- Sweaty feet:Excessive sweating creates ideal conditions for fungal growth.
- Tight or non-breathable footwear: Shoes that trap heat and moisture increase risk.
- Walking barefoot in public areas: Shared showers, locker rooms, and swimming pools are common transmission sites.
- Sharing personal items: Towels, socks, and shoes can spread infection.
- Weakened immune system: Individuals with diabetes or immune disorders may be more susceptible.
- Minor skin injuries: Cracks, cuts, or blisters allow fungi to enter the skin more easily.
Types of Athlete’s Foot
Athlete’s foot does not always look the same. It can appear in different forms:
1. Interdigital Type (Between the Toes)
- Most common type
- Typically occurs between the fourth and fifth toes
- Causes itching, scaling, and cracked skin
2. Moccasin Type
- Affects the soles and sides of the feet
- Skin becomes dry, thickened, and scaly
- May spread to toenails
3. Vesicular Type
- Characterized by fluid-filled blisters
- Often appears on the soles
- May cause burning sensation
4. Ulcerative Type
- Rare but severe
- Open sores and secondary bacterial infection may occur
- More common in people with diabetes
Symptoms of Athlete’s Foot
Symptoms vary depending on the type and severity of infection. Common signs include:
- Itching, especially after removing shoes
- Burning or stinging sensation
- Redness and inflammation
- Cracked or peeling skin
- Scaly patches
- White, soggy skin between toes
- Blisters
- Dry, flaky skin on soles
- Foul odor
- Thickened or discolored toenails (if infection spreads)
In some cases, symptoms may be mild and go unnoticed until the infection worsens.
How Athlete’s Foot Spreads?
Athlete’s foot is contagious and spreads through:
- Direct skin-to-skin contact
- Contact with contaminated surfaces
- Sharing towels or footwear
- Wearing infected shoes or socks
The fungi can survive on surfaces for extended periods, making public spaces common transmission areas.
Diagnosis of Athlete’s Foot
In many cases, a doctor can diagnose athlete’s foot by examining the affected skin. If the diagnosis is uncertain, a skin scraping may be taken and examined under a microscope or sent to a laboratory to confirm fungal infection.
Treatment for Athlete’s Foot
Treatment options depends on severity and duration. Early treatment typically leads to quicker recovery.
1. Over-the-Counter Antifungal Medications
These include creams, sprays, powders, and ointments containing:
- Clotrimazole
- Miconazole
- Terbinafine
- Tolnaftate
Treatment usually lasts 2 to 4 weeks. It’s important to continue applying medication for the full recommended duration—even if symptoms improve earlier.
2. Prescription Medications
For persistent or severe infections, doctors may prescribe:
- Stronger topical antifungal creams
- Oral antifungal medications (e.g., terbinafine or itraconazole)
Oral medications may be necessary if the infection spreads to toenails.
3. Treating Secondary Infections
If bacterial infection develops, antibiotics may be required.
4. Antifungal Powders and Sprays
Antifungal powders and sprays help treat the infection while keeping the feet dry. They are especially useful for people who sweat heavily or need a preventive option inside shoes.
5. Combination Antifungal and Steroid Creams
In cases with severe redness and inflammation, doctors may prescribe creams that combine antifungal medication with a mild corticosteroid. These reduce itching and swelling while treating the fungus, but they are usually recommended for short-term use.
6. Oral Antifungal Medications
For stubborn, widespread, or recurring infections, doctors may prescribe oral antifungals such as terbinafine, itraconazole, or fluconazole. These medications work from inside the body and are often used when the infection spreads to toenails.
7. Antifungal Nail Treatments
If the fungus spreads to the toenails, medicated nail lacquers or oral antifungal drugs may be required. Nail infections take longer to treat and may need several months of therapy.
8. Medicated Foot Soaks
Some doctors recommend prescription-strength antifungal soaks or solutions to help reduce fungal load before applying creams. These can improve treatment effectiveness.
9. Treatment for Secondary Bacterial Infection
If cracks in the skin allow bacteria to enter, antibiotics may be prescribed. Signs include swelling, pus, warmth, or increased pain.
10. Shoe and Sock Disinfection
Treating athlete’s foot is not complete without disinfecting footwear. Antifungal sprays for shoes, washing socks in hot water, and allowing shoes to dry fully help prevent reinfection.
11. Moisture-Control Strategies
Since fungus thrives in damp environments, moisture control is part of treatment. This includes:
- Using moisture-wicking socks
- Changing socks twice daily if needed
- Rotating shoes to allow drying
- Using foot powders regularly
12. UV Shoe Sanitizers
Ultraviolet shoe sanitizing devices can reduce fungal contamination inside footwear. These may help people with frequent recurrences.
13. Laser Therapy (For Nail Involvement)
In chronic nail infections related to athlete’s foot, laser treatment may be used in specialized clinics. It targets fungal cells without damaging surrounding tissue.
How to Improve Treatment Success?
- Apply medication to clean, completely dry skin.
- Continue treatment for the full recommended duration, even if symptoms improve.
- Treat both feet if necessary, even if only one appears infected.
- Avoid scratching, which can spread infection.
When Treatment Doesn’t Work?
If athlete’s foot does not improve after 2–4 weeks of consistent treatment, consult a healthcare provider. The condition may be misdiagnosed, resistant to medication, or complicated by another skin disorder. Early, consistent treatment combined with proper hygiene gives the best chance of complete recovery and prevents recurrence.
Home Remedies for Athlete’s Foot
While antifungal medications remain the most effective treatment for Tinea pedis, certain home remedies may help relieve mild symptoms such as itching, burning, and odor. These remedies work best in early or minor cases and should not replace medical treatment for moderate to severe infections.
1. Hydrogen Peroxide Soak
Hydrogen peroxide may help kill surface bacteria and some fungi. Mix equal parts hydrogen peroxide and warm water, soak your feet for 10–15 minutes, then dry thoroughly.
2. Epsom Salt Soak
Epsom salt can help reduce inflammation and dry out blisters. Dissolve half a cup of Epsom salt in warm water and soak feet for 15–20 minutes daily.
3. Black Tea Soak
Black tea contains tannins that may help reduce fungal growth and sweating. Steep several tea bags in hot water, cool it, and soak feet for about 20 minutes.
4. Neem (Indian Lilac)
Neem leaves or neem oil have antifungal and antibacterial properties. Apply diluted neem oil to the affected area or use boiled neem water as a foot rinse.
5. Aloe Vera
Aloe vera has soothing and mild antifungal effects. Apply fresh aloe gel to clean, dry feet to reduce itching and irritation.
6. Oregano Oil
Oregano oil contains compounds with antifungal properties. Always dilute it with a carrier oil before applying to avoid skin irritation.
7. Cornstarch
Cornstarch helps absorb excess moisture. Apply it between toes to keep the area dry, especially if you sweat heavily.
8. Rubbing Alcohol
Alcohol can help disinfect the skin and dry out moisture. Lightly apply to affected areas and allow it to air dry.
9. Salt Water Soak
Salt water may help dry blisters and reduce infection spread. Mix one teaspoon of salt per cup of warm water and soak for 10–15 minutes.
10. Garlic Paste
Garlic contains allicin, which may have antifungal effects. Crush fresh garlic, mix with a little olive oil, apply briefly to the skin, and rinse after 10–15 minutes.
11. Tea Tree Oil
Has natural antifungal properties. Should be diluted before use.
12. Vinegar Soaks
Soaking feet in diluted vinegar may help reduce fungal growth.
13. Baking Soda
Can help absorb moisture and reduce odor.
Important Tips When Using Home Remedies
- Always dry your feet thoroughly after soaking.
- Test a small area first to avoid allergic reactions.
- Stop using any remedy that causes irritation or worsening symptoms.
- If symptoms persist beyond two weeks, seek medical advice.
Home remedies can provide supportive relief, but consistent foot hygiene and proper antifungal treatment remain the most reliable ways to eliminate athlete’s foot completely. These remedies may provide relief but should not replace antifungal medications in moderate to severe cases.
How Long Does Athlete’s Foot Last?
- Mild cases: 1 to 2 weeks with treatment
- Moderate cases: 2 to 4 weeks
- Severe or untreated cases: Several months
Stopping treatment too early can cause recurrence.
Complications of Athlete’s Foot
If left untreated, athlete’s foot can lead to complications:
1. Spread to Toenails
Fungal infection of the nails can become harder to treat.
2. Spread to Other Body Parts
Infection can spread to hands, groin, or other skin areas.
3. Bacterial Infection
Cracked skin may allow bacteria to enter, leading to cellulitis.
4. Chronic Recurrence
Repeated infections may occur in humid climates.
People with diabetes should seek medical attention early, as foot infections can become serious.
Athlete’s Foot and Diabetes
Individuals with diabetes are at higher risk for complications. Poor circulation and reduced sensation in the feet can delay detection of infection. Untreated fungal infections can lead to serious complications, including ulcers.
Diabetic individuals should:
- Inspect feet daily
- Seek medical care at first signs of infection
- Avoid self-treatment without medical advice
How to Prevent Athlete’s Foot?
Preventing athlete’s foot is often easier than treating it.
1. Keep Feet Clean and Dry
- Wash feet daily
- Dry thoroughly, especially between toes
2. Wear Breathable Footwear
- Choose shoes made of natural materials
- Alternate shoes daily to allow drying
3. Change Socks Daily
- Use moisture-wicking socks
- Change socks if they become damp
4. Avoid Walking Barefoot in Public
- Wear flip-flops in showers and pool areas
5. Use Antifungal Powder
- Especially if prone to sweating
6. Don’t Share Personal Items
- Avoid sharing towels, shoes, or socks
7. Trim Toenails Properly
- Keep nails short and clean
Athlete’s Foot in Children
Although more common in adults, children can develop athlete’s foot. It is less frequent before puberty but can occur if children:
- Participate in sports
- Wear tight shoes
- Use communal changing areas
Treatment is similar to adults, but parents should consult a pediatrician before using strong medications.
Athlete’s Foot vs. Other Foot Conditions
Some conditions resemble athlete’s foot:
Eczema
Usually less contagious and often linked to allergies.
Psoriasis
May cause thick, scaly skin but typically affects other areas too.
Contact Dermatitis
Caused by irritation from soaps or footwear.
Proper diagnosis ensures correct treatment.
When to See a Doctor?
Consult a healthcare provider if:
- Symptoms do not improve after 2 weeks of treatment
- Infection spreads
- Severe redness or swelling occurs
- Pus or fever develops
- You have diabetes
- The infection keeps returning
Early medical intervention prevents complications.
Can Athlete’s Foot Go Away on Its Own?
In rare cases, mild infections may improve, but most cases require treatment. Without antifungal medication, the infection often persists or worsens.
Is Athlete’s Foot Contagious?
Yes. It spreads easily in shared environments. Proper hygiene and preventive measures are essential to avoid transmission.
Can You Exercise with Athlete’s Foot?
Yes, but take precautions:
- Keep feet clean and dry
- Change socks immediately after exercise
- Disinfect footwear
- Avoid sharing equipment
Emotional and Social Impact
Though not life-threatening, athlete’s foot can cause discomfort, embarrassment due to odor, and self-consciousness. Chronic cases may affect confidence and quality of life. Proper treatment and preventive care can restore comfort and confidence.
Final Thoughts
Athlete’s foot may seem like a minor inconvenience, but ignoring it can lead to persistent discomfort and complications. The good news is that it is highly treatable with proper care. Understanding its causes, recognizing early symptoms, and following preventive measures can protect your feet and overall health.
FAQ’s
Can athlete’s foot spread to other body parts?
Yes, it can spread to the nails, hands, or groin. Proper hygiene helps prevent spreading.
What does athlete’s foot look like?
It often appears as red, scaly, or cracked skin. Blisters may develop in some cases.
Is athlete’s foot dangerous?
It is usually mild but can cause complications if untreated. People with diabetes should be cautious.
Can children get athlete’s foot?
Yes, especially if they use shared sports facilities. It is more common in adults than children.
How can I prevent athlete’s foot from returning?
Keep your feet clean and dry daily. Wear breathable shoes and change socks regularly.
How do you get athlete’s foot?
By contact with fungal spores in moist environments like locker rooms or from contaminated surfaces.
Can athlete’s foot spread to hands?
Yes. Scratching infected feet can transfer fungi to hands.
Does athlete’s foot smell?
Yes, fungal growth and bacterial involvement can cause unpleasant odor.
Is athlete’s foot ringworm?
Yes, athlete’s foot is a type of ringworm infection. It is medically called Tinea pedis and is caused by dermatophyte fungi.
What can be mistaken for athlete’s foot?
Conditions like eczema, psoriasis, contact dermatitis, or bacterial infections can look similar. A proper diagnosis helps ensure correct treatment.
Does coconut oil heal athlete’s foot?
Coconut oil has mild antifungal properties and may soothe irritation. However, it is usually not strong enough to completely cure a fungal infection on its own.
Can too much sugar cause athlete’s foot?
Sugar does not directly cause athlete’s foot. However, high blood sugar levels, especially in people with diabetes, can increase the risk of infections.
What food should be avoided with athlete’s foot?
There is no specific diet that causes or cures athlete’s foot. Maintaining a balanced diet and controlling blood sugar levels supports overall immune health.
Also Read: