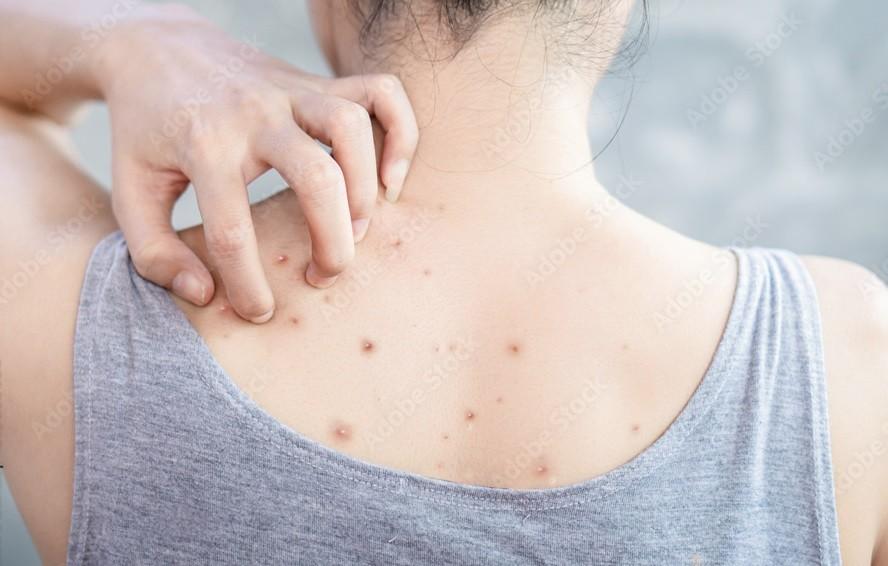
Back acne—often called “bacne”—is one of the most frustrating skin problems for teenagers and adults alike. It hides under clothing but can hurt, itch, and stain your confidence every time you slip into a backless dress or tank top. And unlike facial acne, it is much harder to see, reach, and treat consistently.
If you have ever avoided the beach, the gym, or even certain outfits because of the way your back looks, you are not alone. Back acne is incredibly common, and it affects millions of people worldwide. The good news is: it is manageable, treatable, and in many cases preventable.
In this guide, we will walk you through everything you need to know about back acne — from what causes it and why it happens on the back specifically, to the best treatment options, natural remedies, and lifestyle changes that actually work.
What Is Back Acne?
Back acne is a type of acne that appears on the skin of your back, including the upper back, mid-back, lower back, and even the shoulders. Just like facial acne, it forms when:
- Hair follicles become clogged with oil (sebum) and dead skin cells
- Bacteria multiply inside the blocked pores
- Inflammation develops, forming pimples, whiteheads, blackheads, cysts, or painful nodules
However, the skin on your back is thicker than the skin on your face and has more oil-producing glands. That makes it even more prone to clogged pores and breakouts.
Back acne can show up as:
- Small red bumps
- Whiteheads or blackheads
- Painful cysts
- Large inflamed pimples
- Dark spots or scars (after acne heals)
For some people, it’s occasional. For others, it is chronic and persistent, lasting for years.
Why Does Back Acne Happen?
One of the biggest mistakes people make is thinking that back acne is only caused by poor hygiene. In reality, the reasons are much more complex and often unrelated to how clean you are.
Here are the main causes of back acne:
1. Excess Oil Production
Your back contains many sebaceous (oil) glands. When these glands produce too much oil, it mixes with dead skin cells and clogs your pores. This creates a perfect environment for acne-causing bacteria to grow.
2. Sweat and Friction
Sweating is natural, but when sweat remains on your skin for too long, it mixes with bacteria and oil. Add friction from tight clothing, backpack straps, bras, or sports equipment, and your pores become irritated and inflamed.
This is why people who exercise frequently or live in hot, humid climates are more prone to bacne.
3. Hormonal Changes
Hormonal fluctuations, especially during puberty, menstruation, pregnancy, or stress, can increase oil production in your skin. This is one of the most common reasons why teenagers and young adults suffer from back acne.
Hormonal imbalances such as Polycystic Ovary Syndrome (PCOS) can also make bacne worse in women.
4. Poor Shower Habits After Sweating
Leaving sweat on your skin after a workout or long day can clog pores. Many people forget to shower immediately after exercise or forget to properly clean their back area.
Even if you shower daily, if you don’t clean your back effectively, residue can build up.
5. Hair Products
Shampoos, conditioners, hair oils, and styling gels can run down your back while bathing. These products often contain heavy oils and silicones that clog pores and trigger breakouts along the upper back and shoulders.
6. Cell Phone and Backpack Bacteria
Straps from backpacks or repeated contact with contaminated surfaces can introduce bacteria and irritate the skin continuously, creating breakouts over time.
7. Stress
High stress levels release cortisol, a hormone that stimulates oil glands. Stress won’t directly “cause” acne, but it can definitely make it worse and more difficult to heal.
Types of Back Acne
Back acne is not just one single type of breakout. It shows up in different forms, and each type behaves in its own way. Understanding what kind of back acne you have is the first step toward choosing the right treatment.
1. Comedonal Acne (Non-Inflammatory)
This is the mildest form of back acne and is mainly caused by clogged pores.
It includes:
- Blackheads – Open pores filled with oil and dead skin that appear black on the surface.
- Whiteheads – Closed pores that form small, flesh-colored or white bumps.
Comedonal acne does not usually hurt, but it can make the back look bumpy and uneven.
2. Papules (Inflamed Small Bumps)
Papules are small, red, raised bumps without any visible pus. They appear when the clogged pore becomes irritated and inflamed.
How it feels:
- Tender to touch
- Slightly itchy or uncomfortable
- Often appear in clusters
This type is more noticeable than blackheads and whiteheads.
3. Pustules (Pus-Filled Pimples)
Pustules are what most of us recognize as typical pimples. These are red at the base and have a white or yellow center filled with pus.
Common signs:
- Painful or sensitive
- More inflamed than papules
- Risk of scarring if popped
These are common in moderate back acne.
4. Nodules (Hard, Painful Lumps)
Nodules form deep under the skin and are solid, painful lumps. They are caused by severe inflammation deep inside the pores.
Important to know:
- They are hard and painful
- Take a long time to heal
- Almost always leave marks or scars
- Cannot be treated with home remedies alone
Nodular acne usually needs medical treatment.
5. Cysts (Severe, Deep Acne)
Cystic acne is the most severe form of back acne. It forms large, pus-filled, soft lumps that are deep under the skin.
Features include:
- Very painful
- Highly inflamed
- Often connected under the skin
- High risk of permanent scarring
Cystic back acne requires treatment from a dermatologist.
6. Fungal Acne (Malassezia Folliculitis)
Sometimes back acne is not actually acne but a fungal infection of the hair follicles.
How it looks:
- Small, uniform bumps
- Often itchy
- Appears on the upper back and shoulders
- Gets worse with sweat and humidity
This type does not respond to regular acne treatments and needs antifungal products instead.
7. Hormonal Back Acne
This type is caused by hormonal imbalances, especially in teenagers, women during menstrual cycles, pregnancy, PCOS, or periods of high stress.
Signs:
- Deep, painful pimples
- Appears mainly on shoulders and along the spine
- Breakouts appear in cycles
Treating the hormone imbalance is key here.
8. Mechanical Back Acne (Acne Mechanica)
This type develops due to friction, pressure, and heat trapped against the skin.
Common causes:
- Tight clothing
- Sports gear
- Backpacks
- Sitting for long periods
The constant rubbing irritates hair follicles and worsens acne.
How Back Acne Differs from Facial Acne
While the basic causes are the same, the back is more difficult to treat because:
- The skin is thicker
- Clothing constantly rubs against it
- It’s hard to reach and clean properly
- Healing takes longer
- Scarring is more likely due to deep inflammation
This is why your regular facial cleanser may not be enough to treat bacne.
Treatments for Back Acne
Treating back acne takes consistency and the right combination of ingredients, habits, and sometimes professional help. Because the skin on the back is thicker and produces more oil than the face, it usually needs stronger and more targeted treatments to see real improvement.
1. Medicated Body Washes
One of the easiest and most effective ways to treat back acne is by using the right body wash daily.
These ingredients work best:
- Salicylic Acid (1–2%) – Unclogs pores and removes dead skin cells.
- Benzoyl Peroxide (5–10%) – Kills acne-causing bacteria and reduces inflammation.
- Glycolic Acid – Gently exfoliates the skin and improves texture over time.
How to use:
Apply the body wash to your back, leave it on for 1–2 minutes, then rinse thoroughly. This gives the active ingredients enough time to work.
2. Topical Treatments (Creams & Gels)
These are applied directly to the affected area after showering:
- Retinoid creams or gels – Increase cell turnover and prevent clogged pores.
- Antibiotic creams – Reduce bacteria and inflammation.
- Azelaic acid – Calms redness and improves dark spots over time.
These treatments are especially useful for mild to moderate back acne.
3. Oral Medications (Prescription Only)
For more severe or cystic back acne, a dermatologist may prescribe:
- Oral antibiotics – To reduce bacteria and inflammation
- Hormonal treatments – Often used in women with hormonal acne or PCOS
- Isotretinoin (Accutane) – For very severe or stubborn cases
These treatments should always be taken under medical supervision due to possible side effects.
4. Chemical Peels
Chemical peels containing salicylic acid, glycolic acid, or lactic acid can help:
- Unclog pores
- Reduce active acne
- Fade acne scars
- Smooth rough skin
These are usually done by professionals, but at-home peels are also available (with caution).
5. Laser and Light Therapy
Laser treatments kill acne-causing bacteria and reduce oil gland activity. They are effective for:
- Chronic or severe back acne
- Deep acne scars
- Uneven skin texture
Multiple sessions are usually needed for best results.
6. Treatment for Back Acne Scars
If acne has already left marks or scars, these options can help:
- Vitamin C serums
- Retinol creams
- Micro-needling
- Chemical peels
- Laser treatments
The earlier you treat acne, the less likely it is to scar.
20 Best Home Remedies for Back Acne
Back acne can be stubborn, but nature offers several gentle and powerful solutions. These remedies help reduce oil, fight bacteria, calm inflammation, and support healing when used consistently.
1. Aloe Vera Gel
Aloe vera is soothing, antibacterial, and anti-inflammatory. Apply fresh aloe gel directly to your back after showering. Do not rinse.
2. Tea Tree Oil
Tea tree oil fights acne-causing bacteria. Mix 3–4 drops with a carrier oil like coconut or jojoba oil and apply it to the acne-affected areas.
3. Apple Cider Vinegar
Dilute apple cider vinegar with water (1:3). Apply with a cotton pad to balance skin’s pH and kill bacteria. Rinse after 10 minutes.
4. Neem Leaves or Neem Oil
Neem is a powerful natural antibacterial agent. Apply neem oil or use neem-infused water on your back to reduce infection.
5. Green Tea Spray
Brew green tea, let it cool, and spray onto your back daily. It reduces inflammation and oil production.
6. Turmeric Paste
Turmeric has strong anti-inflammatory and antibacterial properties. Mix turmeric with water or honey and apply for 10–15 minutes.
7. Honey
Raw honey is naturally antibacterial. Apply a thin layer to the back and rinse after 20 minutes.
8. Multani Mitti (Fuller’s Earth)
Multani mitti absorbs excess oil and cleans pores. Mix with rose water, apply as a pack once or twice a week.
9. Baking Soda (Use Occasionally)
Mix with water for a gentle exfoliating paste. Use once a week to remove dead skin cells. Do not overuse.
10. Coconut Oil (For Dry Skin Only)
Coconut oil has antibacterial properties but may clog pores for oily skin. Use a small amount on dry or irritated skin.
11. Lemon Juice
Lemon contains natural acids that kill bacteria. Apply diluted lemon juice for 5–10 minutes. Avoid sun exposure after using it.
12. Oats Scrub
Ground oats mixed with yogurt form a gentle exfoliating and soothing scrub for the back.
13. Epsom Salt Bath
An Epsom salt bath helps draw out toxins, reduce inflammation, and relax the skin.
14. Cucumber Juice
Cucumber cools irritated skin. Apply freshly extracted juice for hydration and calming effects.
15. Witch Hazel
Witch hazel tones skin and reduces oil. Apply it to the back with a cotton pad daily.
16. Garlic Extract (Spot Treatment)
Garlic has antimicrobial properties. Rub a sliced garlic clove gently over pimples (use with caution to avoid irritation).
17. Fenugreek (Methi) Paste
Fenugreek helps reduce swelling and bacteria. Grind soaked seeds into a paste and apply.
18. Sandalwood Powder Paste
Mix sandalwood with water or rosewater. It cools the skin and reduces inflammation.
19. Yogurt
Rich in probiotics and lactic acid, yogurt gently exfoliates and restores skin balance. Apply as a mask.
20. Tomato Pulp
Tomato pulp helps reduce excess oil. Apply the pulp on the back and rinse after 15 minutes.
Important Tips When Using Home Remedies
- Always do a patch test first
- Start slowly and observe how your skin reacts
- Avoid mixing too many remedies at once
- Be consistent for at least 4–6 weeks
- Do not apply on open or bleeding pimples
Home remedies work best for mild to moderate back acne and should be combined with proper hygiene, a healthy diet, and stress management for best results.
How to Prevent Back Acne?
Prevention is always better than cure. Here is how to protect your back from future breakouts:
- Shower immediately after sweating
- Wear loose, breathable cotton clothing
- Change sweaty clothes as soon as possible
- Wash your back last when showering to remove conditioner residue
- Avoid heavy, oily skincare products on your back
- Use a clean towel every time
- Wash bed sheets and pillowcases weekly
- Clean backpacks and gym gear regularly
Consistency with these habits can drastically reduce new breakouts.
Diet Tips for Clearer Skin
Your skin reflects what you eat. A poor diet can make back acne worse.
Try to increase:
- Fresh fruits and vegetables
- Whole grains
- Lean protein
- Omega-3 fatty acids (nuts, seeds, fish)
- Plenty of water
Try to reduce:
- Sugary foods and soft drinks
- Dairy products (for some people)
- Deep-fried foods
- Highly processed snacks
Many people see visible improvement in their skin within a few weeks of eating cleaner.
Can Back Acne Leave Scars?
Yes, unfortunately, back acne can leave behind:
- Deep scars
- Dark spots (hyperpigmentation)
- Uneven skin texture
Scarring happens when inflammation damages the deeper layers of the skin. This is why it’s important not to pick, scratch, or pop back pimples.
Once scars form, treatment options include chemical peels, microneedling, laser therapy, and topical creams recommended by dermatologists.
When Should You See a Doctor?
You should consult a dermatologist if:
- Your back acne is severe and painful
- It keeps spreading
- It leaves dark scars
- Over-the-counter treatments don’t help
- It affects your self-confidence or mental health
A professional can customize a treatment plan for you and prevent long-term damage.
Mental and Emotional Impact of Back Acne
Back acne doesn’t just affect your skin—it can deeply impact how you feel about yourself. Many people feel embarrassed, avoid social situations, or struggle with low self-esteem.
If this sounds like you, please remember:
You are not defined by your skin condition.
Back acne is a medical issue, not a personal failure. With the right treatment and patience, your skin can improve.
Confidence comes not from perfect skin, but from understanding that your worth is far greater than any temporary condition.
Final Thoughts
Back acne is common, treatable, and nothing to feel ashamed about. While it may take time, consistency is the key. Start with simple changes: a better shower routine, proper products, and a balanced diet. If needed, seek professional help. Your skin deserves care, patience, and love. Clear skin is not an overnight miracle—it’s a journey. And every small step you take today is bringing you closer to healthier, happier skin.
FAQ’s
How can I get rid of back acne fast?
To get rid of back acne faster, shower after sweating, use a salicylic acid or benzoyl peroxide body wash, wear loose cotton clothing, and avoid picking pimples. For severe cases, consult a dermatologist for prescription treatment.
Is back acne common in adults?
Yes, back acne is common in adults, especially those with hormonal imbalances, high stress levels, or oily skin. It can continue even after teenage years.
Does diet affect back acne?
Yes, a diet high in sugar, processed foods, and dairy can worsen back acne in some people. Eating more fruits, vegetables, lean proteins, and drinking plenty of water can help improve skin health.
Can back acne leave scars?
Yes, severe or untreated back acne can leave permanent scars and dark spots. Avoid popping pimples and treat breakouts early to reduce the risk of scarring.
What is the best body wash for back acne?
Body washes that contain salicylic acid or benzoyl peroxide are considered the best for treating and preventing back acne.
Can stress cause back acne?
Stress increases cortisol levels in the body, which can trigger more oil production and worsen acne on the back.
How long does it take for back acne to clear?
With consistent treatment and proper skincare, mild back acne can start improving within 4 to 6 weeks. Severe cases may take longer and may require medical treatment.
Is back acne hormonal?
Yes, back acne is often linked to hormonal changes. When hormones like androgens increase, your skin produces more oil, which can clog pores and lead to breakouts on the back. This is common during puberty, menstrual cycles, pregnancy, PCOS, or periods of high stress.
Does back acne mean PCOS?
Not always. While back acne can be a symptom of PCOS in some people, it does not automatically mean you have the condition. PCOS usually comes with other signs like irregular periods, excessive hair growth, and weight gain. If back acne is severe and persistent along with these symptoms, it’s best to consult a doctor.
Which deficiency causes back acne?
Certain nutrient deficiencies—especially zinc, vitamin A, vitamin D, and omega-3 fatty acids—can make the skin more prone to acne and inflammation. These nutrients help control oil production, reduce bacteria, and support skin repair.
What vitamin gets rid of back acne?
There is no single vitamin that completely cures back acne, but vitamin A (retinoids), vitamin C, vitamin D, and zinc play an important role in controlling oil, boosting immunity, and repairing the skin. These vitamins can support clearer skin when combined with proper treatment.
What foods help back acne?
Foods that support clear skin include fruits, vegetables, whole grains, nuts, seeds, green tea, fatty fish, and foods rich in antioxidants. These foods help reduce inflammation and regulate hormones, which can prevent future breakouts.
Is back acne genetic?
Yes, genetics can influence whether you are more prone to back acne. If your parents struggled with body acne, oily skin, or hormonal acne, chances are higher that you may experience it too. However, good skincare and lifestyle habits can greatly reduce its severity.
Also Read: