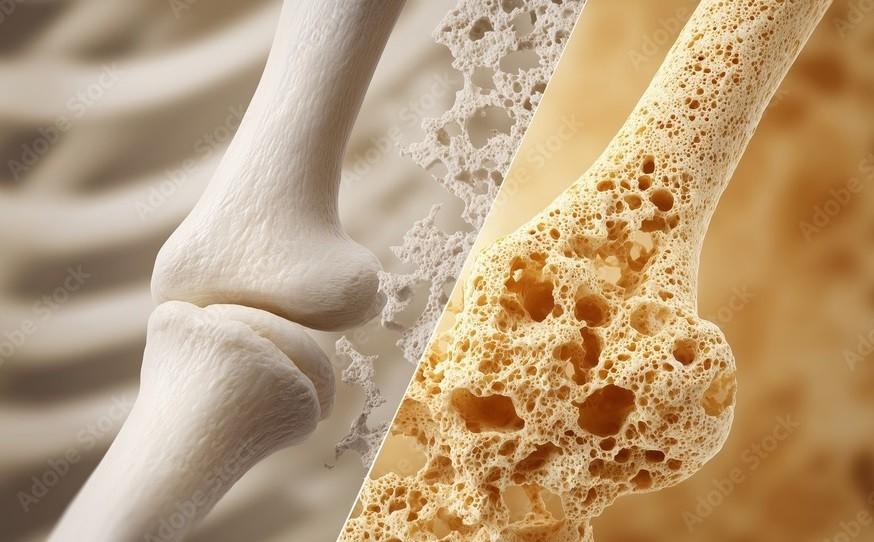
Bone health often goes unnoticed—until a fracture occurs. Many people believe bone problems only affect older adults with osteoporosis, but there is an important stage that often comes first: osteopenia. Osteopenia is not a disease in itself; rather, it is a warning sign. It indicates that your bone mineral density is lower than normal, but not yet low enough to be classified as osteoporosis.
If you’ve recently been diagnosed with osteopenia after a bone density test, you might feel confused or even anxious. What does this mean? Is it reversible? Will it turn into osteoporosis? The good news is that osteopenia is manageable, and in many cases, progression can be slowed or prevented with proper care. In this guide, we will explore everything you need to know about osteopenia—its causes, risk factors, symptoms, diagnosis, treatment options, diet, exercise, and preventive strategies to maintain strong bones for life.
What Is Osteopenia?
Osteopenia refers to reduced bone mineral density (BMD) compared to normal levels. Bone mineral density measures how much calcium and other minerals are present in your bones. These minerals give bones their strength and structure.
Bone density is measured using a DEXA (dual-energy X-ray absorptiometry) scan. Results are expressed as a T-score:
- Normal bone density: T-score of -1.0 or above
- Osteopenia: T-score between -1.0 and -2.5
- Osteoporosis: T-score of -2.5 or lower
Osteopenia indicates that bones are beginning to lose strength. While fractures are less common than in osteoporosis, the risk is higher than in individuals with normal bone density.
How Bone Loss Happens?
Bone is living tissue. Throughout life, your body constantly breaks down old bone (resorption) and builds new bone (formation). This process is known as bone remodeling.
During childhood and early adulthood, bone formation outpaces bone loss. Peak bone mass is typically reached around age 30. After that, bone resorption gradually exceeds bone formation, leading to a slow decline in bone density. In osteopenia, this balance has shifted slightly toward bone loss, but not severely enough to meet the criteria for osteoporosis.
Causes of Osteopenia
Osteopenia develops due to a combination of natural aging and specific risk factors. Common causes include:
1. Aging
As we age, bone formation slows down, and bone resorption increases.
2. Hormonal Changes
Estrogen plays a major role in maintaining bone density. After menopause, estrogen levels drop sharply, accelerating bone loss in women. Similarly, low testosterone levels in men can contribute to bone thinning.
3. Nutritional Deficiencies
Insufficient calcium and vitamin D intake weakens bone structure over time.
4. Sedentary Lifestyle
Bones need weight-bearing activity to stay strong. Lack of exercise contributes to bone loss.
5. Smoking and Excessive Alcohol
Both interfere with bone formation and reduce calcium absorption.
6. Certain Medications
Long-term use of corticosteroids (like prednisone), some anticonvulsants, and certain cancer treatments can reduce bone density.
7. Medical Conditions
- Thyroid disorders
- Rheumatoid arthritis
- Celiac disease
- Chronic kidney disease
- Hormonal disorders
Risk Factors for Osteopenia
Some people are more likely to develop osteopenia. Risk factors include:
- Female gender
- Age over 50
- Family history of osteoporosis
- Low body weight
- Early menopause
- Eating disorders
- Limited sun exposure
- Sedentary lifestyle
- Smoking
- Excessive alcohol consumption
Men can also develop osteopenia, although it is more common in women.
Symptoms of Osteopenia
One of the most challenging aspects of osteopenia is that it usually has no symptoms. There is no pain or obvious warning sign.
Most people discover they have osteopenia after:
- A routine bone density test
- A minor fracture from a low-impact injury
- Screening due to age or risk factors
Because it is silent, early detection through screening is essential.
Diagnosis of Osteopenia
Bone Density Test (DEXA Scan)
The DEXA scan is the gold standard for diagnosing osteopenia. It is painless, quick, and uses minimal radiation.
The scan measures bone density at key areas such as:
- Hip
- Spine
- Forearm
The result provides a T-score that compares your bone density to that of a healthy young adult.
FRAX Score
Doctors may also use the FRAX tool (Fracture Risk Assessment Tool) to estimate your 10-year risk of fracture. It considers factors like age, gender, weight, medical history, and lifestyle.
Osteopenia vs. Osteoporosis
Understanding the difference between osteopenia and osteoporosis is important:
| Feature | Osteopenia | Osteoporosis |
|---|---|---|
| Bone density | Mildly low | Severely low |
| T-score | -1.0 to -2.5 | -2.5 or lower |
| Fracture risk | Moderate | High |
| Treatment urgency | Lifestyle focus | Often medication required |
Osteopenia is a warning stage. With intervention, progression to osteoporosis can often be prevented.
Can Osteopenia Be Reversed?
In some cases, bone density can improve with proper treatment, especially in younger individuals. However, the main goal is usually to prevent further bone loss and reduce fracture risk. Early intervention makes a significant difference.
Treatment of Osteopenia
Treatment depends on:
- T-score
- Age
- Fracture history
- Overall fracture risk
1. Lifestyle Changes
For many people with osteopenia, lifestyle modification is the first line of treatment.
2. Calcium and Vitamin D Supplementation
- Adults generally need 1,000–1,200 mg of calcium per day.
- Vitamin D requirements are usually 800–1,000 IU per day.
These help support bone formation and calcium absorption.
3. Medications
Medications are not always necessary for osteopenia. However, if fracture risk is high, doctors may prescribe:
- Bisphosphonates
- Hormone therapy
- Selective estrogen receptor modulators (SERMs)
Best Diet for Osteopenia
Nutrition plays a central role in bone health.
Calcium-Rich Foods
- Milk and dairy products
- Yogurt
- Cheese
- Leafy greens (kale, spinach)
- Almonds
- Tofu
- Sardines
Vitamin D Sources
- Sunlight exposure
- Fatty fish (salmon, mackerel)
- Egg yolks
- Fortified cereals and milk
Other Important Nutrients
- Magnesium
- Vitamin K
- Protein
- Phosphorus
A balanced diet helps maintain bone density and overall health.
Best Exercises for Osteopenia
Exercise strengthens bones and reduces fall risk.
Weight-Bearing Exercises
- Walking
- Jogging
- Dancing
- Stair climbing
Strength Training
- Resistance bands
- Weightlifting
- Bodyweight exercises
Balance and Flexibility
- Yoga
- Tai Chi
Regular exercise stimulates bone remodeling and slows bone loss.
Lifestyle Tips to Prevent Osteopenia Progression
- Quit smoking
- Limit alcohol consumption
- Maintain a healthy body weight
- Get regular bone density tests
- Prevent falls at home
- Use proper footwear
- Improve home lighting
Osteopenia in Women
Women are at higher risk due to hormonal changes, especially after menopause. Estrogen decline accelerates bone resorption.
Women should consider:
- Early screening after menopause
- Hormone level evaluation
- Adequate calcium intake
Osteopenia in Men
Although less common, men can develop osteopenia, particularly after age 65. Testosterone levels influence bone density in men. Men with risk factors should not ignore bone health screening.
Osteopenia and Fracture Risk
Common fracture sites include:
- Hip
- Wrist
- Spine
Even minor falls can lead to fractures in weakened bones. Preventive measures are crucial.
When to See a Doctor?
Consult a healthcare provider if you:
- Are over 50 and have not had a bone density test
- Have a family history of osteoporosis
- Experience a fracture after minor trauma
- Have risk factors such as steroid use
Long-Term Outlook
Osteopenia does not guarantee that you will develop osteoporosis. With proactive management, many individuals maintain stable bone density for years. The key lies in early detection, healthy habits, and medical guidance.
Final Thoughts
Osteopenia serves as an important warning sign that your bones need attention. While it may sound alarming at first, it is also an opportunity. With timely lifestyle changes, proper nutrition, regular exercise, and medical guidance, you can protect your bones and significantly reduce the risk of fractures and osteoporosis.
FAQ’s
Is osteopenia the same as osteoporosis?
No, osteopenia is less severe than osteoporosis. It is considered a warning stage before osteoporosis develops.
What is a T-score in osteopenia?
A T-score compares your bone density to that of a healthy young adult. A T-score between -1.0 and -2.5 indicates osteopenia.
How often should I get a bone density test?
People diagnosed with osteopenia are generally advised to repeat the test every 1–2 years. Your doctor may adjust the timing based on your individual risk.
Do I need medication for osteopenia?
Not everyone with osteopenia requires medication. Treatment depends on your fracture risk and overall health profile.
Can young adults develop osteopenia?
Yes, although it is less common. Eating disorders, hormonal imbalances, chronic illnesses, and long-term steroid use can increase risk in younger individuals.
Is osteopenia painful?
Osteopenia itself does not cause pain. Pain typically occurs only if a fracture develops.
Can men get osteopenia?
Yes, men can develop osteopenia, especially after age 65 or if they have low testosterone levels or other risk factors.
Does menopause increase the risk of osteopenia?
Yes, the drop in estrogen levels during menopause accelerates bone loss, increasing the risk of osteopenia and osteoporosis.
Can osteopenia lead to fractures?
Yes, people with osteopenia have a higher fracture risk than those with normal bone density, especially if they fall.
How can I prevent osteopenia from worsening?
Maintain a calcium-rich diet, get enough vitamin D, exercise regularly, avoid smoking, limit alcohol, and follow your doctor’s recommendations for monitoring and treatment.
Is osteopenia serious?
Osteopenia is not as severe as osteoporosis, but it increases the risk of fractures. It should be taken seriously as an early warning sign of bone loss.
Can osteopenia turn into osteoporosis?
Yes, without intervention, osteopenia can progress to osteoporosis over time. Proper lifestyle changes and treatment can reduce this risk.
Also Read: