Inflammatory Bowel Disease (IBD) is a chronic condition that causes persistent inflammation in the digestive tract. It can significantly affect quality of life, but with proper diagnosis, treatment, and lifestyle adjustments, many individuals successfully manage the condition and lead full, active lives. This guide explains what IBD is, its types, symptoms, causes, risk factors, complications, diagnosis, treatment options, diet considerations, and mental health impact.
What Is Inflammatory Bowel Disease (IBD)?
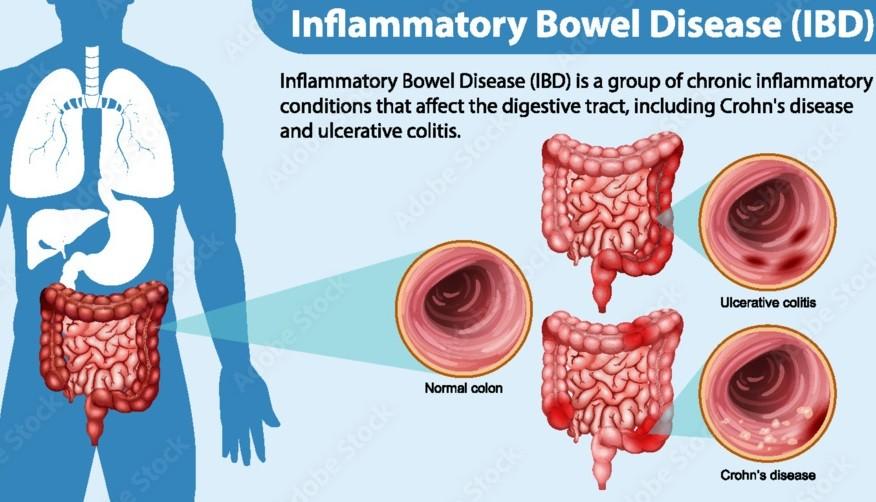
Inflammatory Bowel Disease (IBD) refers to a group of chronic inflammatory conditions that affect the gastrointestinal (GI) tract. The two main types of IBD are:
- Crohn’s disease
- Ulcerative colitis
Both conditions involve abnormal immune responses that lead to ongoing inflammation in the digestive system. IBD is different from Irritable Bowel Syndrome (IBS), which does not cause inflammation or permanent damage to the intestines. Inflammatory Bowel Disease is considered a lifelong condition, characterized by periods of flare-ups (active symptoms) and remission (reduced or no symptoms).
Types of Inflammatory Bowel Disease
1. Crohn’s Disease
Crohn’s disease can affect any part of the digestive tract, from the mouth to the anus. However, it most commonly impacts the end of the small intestine (ileum) and the beginning of the colon.
Key characteristics:
- Inflammation can occur in patches.
- It may affect all layers of the bowel wall.
- It can lead to strictures, fistulas, and abscesses.
2. Ulcerative Colitis
Ulcerative colitis primarily affects the colon (large intestine) and rectum.
Key characteristics:
- Inflammation is continuous rather than patchy.
- It affects only the innermost lining of the colon.
- It may cause ulcers and bleeding.
Causes of Inflammatory Bowel Disease
The exact cause of IBD is not fully understood. However, researchers believe it results from a combination of genetic, immune, and environmental factors.
1. Immune System Dysfunction
IBD is believed to be an autoimmune condition. The immune system mistakenly attacks healthy cells in the digestive tract, causing chronic inflammation.
2. Genetic Factors
People with a family history of IBD have a higher risk of developing the condition. Several genes have been linked to immune regulation and inflammation.
3. Environmental Triggers
Environmental factors may contribute to IBD, including:
- Diet high in processed foods
- Smoking (particularly linked to Crohn’s disease)
- Urban living
- Antibiotic overuse
- Gut microbiome imbalance
4. Gut Microbiome Imbalance
Changes in the balance of bacteria in the intestines may trigger abnormal immune responses in genetically susceptible individuals.
Symptoms of Inflammatory Bowel Disease
Symptoms vary depending on the type and severity of IBD. They may range from mild to severe and can develop gradually or suddenly.
Common Symptoms
- Persistent diarrhea
- Abdominal pain and cramping
- Blood in stool
- Urgency to have bowel movements
- Fatigue
- Weight loss
- Loss of appetite
- Fever (in severe cases)
Additional Symptoms in Crohn’s Disease
- Mouth sores
- Fistulas (abnormal connections between organs)
- Perianal disease (pain or drainage near the anus)
- Malnutrition
Additional Symptoms in Ulcerative Colitis
- Rectal bleeding
- Tenesmus (feeling of incomplete bowel movement)
- Mucus in stool
Extraintestinal Symptoms
Inflammatory Bowel Disease does not only affect the digestive system. It may also cause inflammation in other parts of the body, including:
- Joint pain and arthritis
- Skin conditions (such as erythema nodosum)
- Eye inflammation (uveitis)
- Liver disorders
- Bone density loss
Risk Factors for Inflammatory Bowel Disease
Several factors may increase the risk of developing IBD:
- Family history
- Age (often diagnosed between 15 and 35 years)
- Smoking
- Use of certain medications (NSAIDs)
- Living in industrialized countries
- Diet high in fat and processed foods
Complications of IBD
Without proper treatment, IBD can lead to serious complications.
Complications of Crohn’s Disease
- Intestinal obstruction
- Fistulas
- Abscesses
- Malnutrition
- Anal fissures
Complications of Ulcerative Colitis
- Severe bleeding
- Toxic megacolon
- Perforated colon
- Increased risk of colon cancer
Long-Term Complications
- Osteoporosis
- Anemia
- Vitamin deficiencies (B12, iron, vitamin D)
- Increased colorectal cancer risk
Diagnosis of Inflammatory Bowel Disease
Early and accurate diagnosis is crucial for managing IBD effectively.
1. Medical History and Physical Examination
A doctor will review symptoms, family history, and perform a physical exam.
2. Blood Tests
Blood tests may check for:
- Anemia
- Infection
- Inflammatory markers (CRP, ESR)
3. Stool Tests
Stool samples help rule out infections and detect inflammation markers like calprotectin.
4. Endoscopy and Colonoscopy
A colonoscopy allows direct visualization of the colon and rectum. Biopsies may be taken to confirm diagnosis.
5. Imaging Tests
CT scans and MRI can assess inflammation, complications, and small intestine involvement.
Treatment for Inflammatory Bowel Disease
There is no cure for IBD, but treatments aim to reduce inflammation, relieve symptoms, and maintain remission.
1. Medications
Aminosalicylates (5-ASA)
Used mainly for mild to moderate ulcerative colitis.
Corticosteroids
Used short-term to control flare-ups.
Immunomodulators
Help suppress the immune system to reduce inflammation.
Biologic Therapies
Target specific components of the immune system. Examples include:
- Anti-TNF agents
- Integrin inhibitors
- IL-12/23 inhibitors
JAK Inhibitors
Oral medications that block inflammatory pathways.
2. Surgery
Surgery may be necessary if medications fail or complications arise.
- In Crohn’s disease, surgery removes damaged sections but does not cure the disease.
- In ulcerative colitis, removing the colon (colectomy) can be curative.
Diet and Nutrition in IBD
Diet does not cause IBD, but certain foods may worsen symptoms during flare-ups.
During a Flare-Up
- Low-fiber foods
- Avoid raw vegetables
- Limit dairy if lactose intolerant
- Avoid spicy and fried foods
- Stay hydrated
During Remission
- Balanced diet with fruits and vegetables
- Lean protein sources
- Whole grains (if tolerated)
- Probiotic-rich foods
Nutritional Concerns
People with IBD may require supplements for:
- Iron
- Vitamin B12
- Vitamin D
- Calcium
Consulting a registered dietitian is often helpful.
Lifestyle Changes to Manage IBD
1. Stress Management
Stress does not cause IBD but can worsen symptoms. Helpful strategies include:
- Meditation
- Yoga
- Deep breathing exercises
- Therapy
2. Quit Smoking
Smoking worsens Crohn’s disease and increases flare-ups.
3. Regular Exercise
Moderate physical activity improves digestion, mood, and bone health.
4. Sleep Hygiene
Adequate sleep supports immune regulation and healing.
Mental Health and Inflammatory Bowel Disease
Living with a chronic illness can affect mental well-being. Anxiety and depression are common among people with IBD.
Coping strategies include:
- Support groups
- Counseling
- Cognitive behavioral therapy
- Connecting with others who have IBD
Addressing mental health is essential for overall disease management.
IBD in Children and Adolescents
IBD can develop in children and teens. In pediatric cases, it may affect:
- Growth and development
- Puberty
- Nutritional status
Early treatment is crucial to prevent long-term complications.
Pregnancy and Inflammatory Bowel Disease
Women with IBD can have healthy pregnancies. It is important to:
- Achieve remission before conception
- Continue safe medications
- Work closely with healthcare providers
Active disease during pregnancy may increase risks.
IBD vs IBS: Key Differences
| Feature | IBD | IBS |
|---|---|---|
| Inflammation | Yes | No |
| Intestinal damage | Yes | No |
| Blood in stool | Common | Rare |
| Cancer risk | Increased | No |
| Autoimmune component | Yes | No |
IBS is a functional disorder, while IBD is an inflammatory disease.
Prevention and Early Detection
There is no guaranteed way to prevent Inflammatory Bowel Disease. However:
- Avoid smoking
- Maintain a balanced diet
- Seek early medical evaluation for persistent digestive symptoms
- Follow recommended colon cancer screening if diagnosed
Living Well with Inflammatory Bowel Disease
Managing IBD requires a long-term partnership with healthcare providers. Treatment plans are personalized and may evolve over time. Many individuals with Inflammatory Bowel Disease:
- Work full-time
- Travel
- Exercise regularly
- Have families
Education, early intervention, medication adherence, and lifestyle adjustments play a key role in maintaining remission.
When to See a Doctor?
Seek medical attention if you experience:
- Persistent diarrhea lasting more than a few weeks
- Blood in stool
- Severe abdominal pain
- Unexplained weight loss
- Fever with digestive symptoms
Early diagnosis improves long-term outcomes.
Final Thoughts
Inflammatory Bowel Disease is a complex and lifelong condition that affects millions of people worldwide. Although it presents challenges, advances in medical research have significantly improved treatment options and quality of life for patients.
Understanding the disease, recognizing symptoms early, following medical advice, maintaining a healthy lifestyle, and prioritizing mental well-being are essential components of effective IBD management.
With the right support and treatment plan, individuals with IBD can lead productive, fulfilling lives despite the chronic nature of the condition. If you suspect symptoms of Inflammatory Bowel Disease, consult a healthcare professional for proper evaluation and diagnosis. Early care can prevent complications and help you regain control of your health.
FAQ’s
What is the difference between Crohn’s disease and ulcerative colitis?
Crohn’s disease can affect any part of the digestive tract and may involve all layers of the bowel wall. Ulcerative colitis affects only the colon and rectum and involves inflammation of the inner lining.
Is IBD the same as IBS?
No, IBD and IBS are different conditions. Inflammatory Bowel Disease causes inflammation and structural damage to the intestines, while IBS is a functional disorder without inflammation.
Is IBD hereditary?
Inflammatory Bowel Disease can run in families. Having a close relative with IBD increases the risk, but not everyone with a family history will develop the condition.
Can stress cause IBD?
Stress does not directly cause IBD, but it can trigger or worsen flare-ups. Managing stress may help reduce symptom severity.
What triggers IBD flare-ups?
Common triggers include infections, stress, certain foods, smoking, and stopping medications. Triggers vary from person to person.
Is IBD curable?
There is no cure for Crohn’s disease. Ulcerative colitis may be cured with surgical removal of the colon, but medical treatment typically manages symptoms effectively.
Can IBD go into remission?
Yes, many people experience remission periods where symptoms significantly reduce or disappear. Treatment aims to maintain long-term remission.
Does IBD increase the risk of colon cancer?
Long-standing IBD, especially ulcerative colitis, increases the risk of colorectal cancer. Regular screening colonoscopies are recommended.
Is IBD life-threatening?
Most people with IBD live normal lifespans with proper treatment. However, severe complications can occur if the disease is left untreated.
Can diet cure IBD?
Diet alone cannot cure IBD, but certain dietary changes can help manage symptoms and reduce flare-ups.
What foods should be avoided with IBD?
During flare-ups, people may need to avoid high-fiber foods, spicy dishes, fried foods, dairy (if intolerant), and alcohol. Food tolerances vary individually.
Is IBD contagious?
No, IBD is not contagious. It cannot spread from person to person.
Can children develop IBD?
Yes, IBD can affect children and adolescents. Early diagnosis and treatment are important to support growth and development.
Can someone with IBD live a normal life?
Yes, with proper medical care and lifestyle adjustments, many individuals with IBD lead full and productive lives.
Does smoking affect IBD?
Smoking worsens Crohn’s disease and increases flare-ups and complications. Quitting smoking is strongly recommended.
Are there complications outside the digestive system?
Yes, IBD can affect joints, skin, eyes, and the liver. These are known as extraintestinal manifestations.
How long do IBD flare-ups last?
Flare-ups can last from days to several months, depending on severity and treatment response.
Do all IBD patients need surgery?
Not all patients require surgery. Many manage the disease successfully with medications, but surgery may be necessary if complications develop.
Can probiotics help with IBD?
Probiotics may help some individuals by supporting gut health, but they are not a replacement for medical treatment.
Also Read: